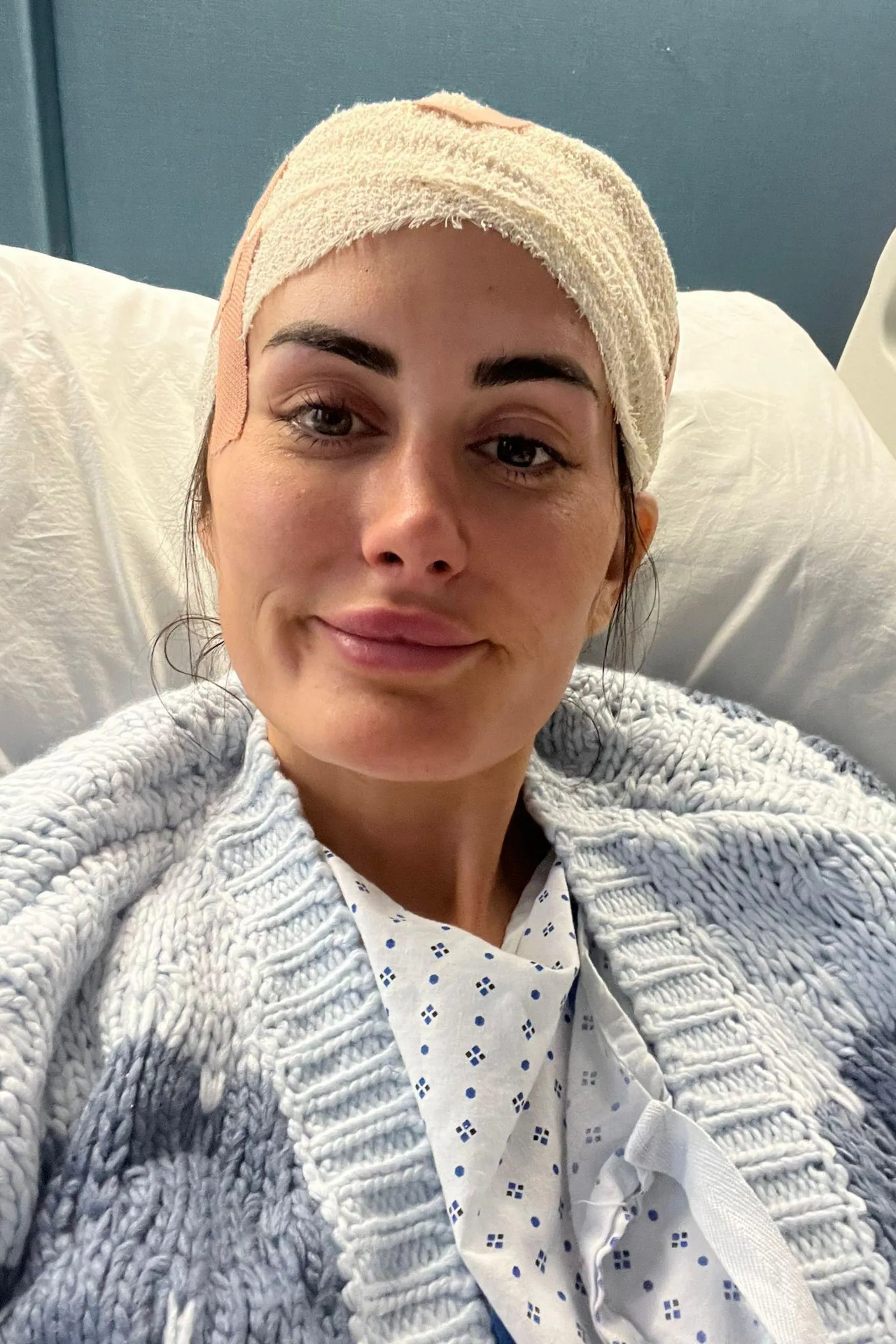
Life-Changing Discovery Following a Train Accident
Lauren Macpherson had planned the August bank holiday weekend as the "first of many" celebrations. She had spent the time at a music festival in London, marking a period of personal achievements including passing exams for a promotion at work and purchasing her first home with her boyfriend, Zak.

However, on her journey home to Cardiff, a 35lb (16kg) suitcase fell from the overhead storage on the train and struck Lauren on the head. This incident led to the unexpected discovery that the 29-year-old had been living with terminal brain cancer.

"We kind of wanted to start celebrating and start living you know," said Lauren, who has been informed she can expect to live for about 10-12 years.
Initial Medical Response and Diagnosis
The impact of the suitcase caused significant swelling, and doctors initially feared Lauren might have a fractured spine. She was taken off the train at Swindon for medical attention, where a CT scan revealed a shadow on her brain.

"I knew straight away," Lauren recalled. "There is an instinct inside you, and when you have been feeling unwell, it just all made sense."
Two days later, an MRI in Cardiff indicated the presence of a brain tumour. Lauren described the moment as almost a relief, providing an explanation for the symptoms she had been experiencing.
"It's almost like a relief, you think you're going crazy, all these things going wrong," she said.
Symptoms and Prior Health Concerns
In the year before the accident, Lauren had been experiencing emotional dysregulation and extreme fatigue, symptoms initially attributed to hormonal changes or undiagnosed ADHD. She visited her GP three times for various tests due to additional issues such as gut problems and blackouts.
The fatigue was severe enough that Lauren reduced her work hours from full-time to part-time as a cardiographer to manage her Master's degree studies.
"To be honest I was quite naive... I was worried but at this point I wasn't scared. I didn't think at this point, it's incurable, I just thought 'they've found it, they can get rid of it'."
Severity of Diagnosis and Treatment Decisions
At a follow-up appointment a month later, the seriousness of Lauren's condition became clear. Doctors suspected glioblastoma, a fast-growing brain tumour, with a prognosis of possibly just two years if aggressive.
"We just had our flat whites, we thought we would be an hour there and go on with our day," Lauren said. "We did not expect it at all. Then it kind of hit me and that's when you're like 'oh my God, you could be looking at two years'."
Lauren was advised she needed surgery to remove the tumour, but NHS waiting times meant a four-month delay. Opting for a quicker option, she accessed a private clinic through her partner Zak's healthcare coverage, reducing the wait to three weeks.
"You feel like there is this disease inside of you and you just want to get it out," she explained. "Even in the consultation, I didn't cry. I didn't not cry because I'm brave, strong and hard... it's not that. But for me, it's almost like you have a survival instinct that kicks in... I wasn't happy, I wasn't sad, I wasn't hopeful."
Impact on Family and Surgery Outcome
The diagnosis was devastating for both Zak and Lauren's family.
Lauren underwent brain surgery at the end of October, which successfully removed approximately 80% of the tumour. A biopsy confirmed a grade two oligodendroglioma, a rare, fast-growing, incurable brain tumour, but at an earlier stage.
"It's almost like somebody had given me a new brain, it was really strange, nothing made sense, I didn't feel like me," Lauren said.
Since the tumour was located in the speech cortex, Lauren was unable to speak for weeks post-surgery and experienced significant cognitive impairment. Her recovery included episodes of sickness and vertigo.
"I underestimated how difficult the first month would be, I just wanted to start feeling OK."
Raising Awareness and Exploring Treatment Options
Seeking connection with others facing similar challenges, Lauren created an Instagram page to raise awareness and document her journey.
"You just want to talk to people and see how everyone else is doing and how other people feel," she said.
Through these connections, Lauren learned about vorasidenib, a less aggressive treatment option for patients who do not require immediate chemotherapy or radiotherapy after surgery.
This treatment is approved under the National Institute for Health and Care Excellence (NICE) guidelines for use on the NHS in Scotland but is not yet available in Wales, England, or Northern Ireland. Lauren is actively campaigning for its availability in these regions.
The Welsh government stated it relies on NICE's independent advice to ensure the cost of treatments made routinely available to patients in Wales is balanced with their benefits.
"While trial evidence shows it can slow cancer progression, there is no clear evidence it helps people live longer," the statement said.
It also noted that NICE had provisionally recommended vorasidenib should not be available on the NHS, with final guidance expected later in the year.
Ongoing Care and Outlook
Lauren requires scans every three months to monitor her tumour and is currently undergoing fertility treatment before beginning vorasidenib therapy, which she is receiving through a private provider.
"Medicine is excelling at a rate it has never done before, AI is taking over as we know, so I'm really hopeful on that front."
While Lauren remains hopeful, she acknowledges the emotional toll of her diagnosis.
"The whole thing has been hard for me... but for family, it's almost been harder for them," she said.
"I think everyone always says 'I wish it was me not you' but I could really see it with them, constantly the pain in their eyes, because they wanted it to be them not me. It was really, really, hard, I wouldn't wish that on anyone, having to deal with that."