Living with the aftermath of anal cancer treatment
A woman diagnosed with anal cancer has revealed the severe pain she continues to endure six years after undergoing pelvic radiotherapy. Trish Prosser, 57, described how her vaginal walls closed over as a result of the treatment, leaving her in constant agony.
Trish, a mother of four, expressed that she initially felt too embarrassed to disclose the nature of her cancer to family and friends due to the stigma associated with anal cancer.
Anal cancer is a rare disease, with approximately 1,500 new cases diagnosed annually in the UK. Of these, around 40 to 50 cases occur in Northern Ireland.
"People are too embarrassed to talk about issues down below or in their bottoms, it can be embarrassing even taboo, but I want to help break the stigma,"
Trish was diagnosed in 2020, coinciding with the onset of the coronavirus pandemic, which she said made her cancer journey particularly isolating. It is only recently that she has felt able to openly discuss the trauma she experienced.
"I may have looked normal on the outside as I didn't lose my hair, but I felt awful on the inside, I just felt I was falling apart,"she said.
"My worst symptom was fatigue; I was so tired. I also had an itch around my anal area, but I had no changes to my bowel habits and to be honest none of those symptoms normally associated with cancer,"Trish added.
Challenges in Northern Ireland's healthcare provision
Unlike other parts of the UK, Northern Ireland currently lacks a dedicated clinic or one-stop service for patients who have undergone pelvic radiotherapy.
Trish, who lives in Belfast, emphasized that surviving cancer treatment is only the initial phase of recovery, which for many patients can span several years.
"There are the physical scars which for those who have pelvic radiotherapy can mean dealing with bowel, vulva, cervical and vaginal scarring which is horrendously painful,"she explained.
"I didn't want people to know what I was going through because it was such a personal area of my body - so when people asked, I just said I'm fine."

What is anal cancer?
Anal cancer primarily results from persistent infection with high-risk strains of the Human Papillomavirus (HPV), which accounts for up to 90% of cases. HPV causes abnormal cell growth in the anal canal, leading to tumour formation.
Other notable risk factors include a weakened immune system and a history of other gynaecological cancers. However, only a small fraction of individuals infected with HPV will develop anal cancer.
Impact of pelvic radiotherapy on intimacy
Pelvic radiotherapy for anal cancer can cause significant and long-lasting vaginal damage due to the close proximity of vaginal tissues to the treatment area. This condition, often referred to as radiation-induced vaginal stenosis, involves the formation of scar tissue that shortens, narrows, dries, and reduces the flexibility of the vagina, potentially causing cuts and tissue damage.
While such effects can occur during treatment, they often persist or emerge months or years after treatment completion.
"I wasn't aware that my vagina had actually stuck together and I needed to open it again and that had to be done through a dilator or intimacy - and intimacy was painful,"Trish said.
"But as you start to recover you start to think about being intimate again and I was so lucky to have a strong loving partner that was patient and helped me through that stage,"she added.

Care beyond treatment
Radiotherapy UK, in collaboration with the gastrointestinal clinical oncology team at Belfast Health and Social Care Trust, is seeking to initiate conversations about anal cancer, which remains one of the most under-discussed cancers.
The goal among charities and healthcare professionals is to establish a comprehensive care pathway that supports patients throughout and beyond their cancer treatment.
Sarah Quinlan of Radiotherapy UK stated:
"Late effects from cancer can emerge months or even years after treatment finishes, significantly affecting quality of life, independence and a person's well-being.
We want a well-resourced, multidisciplinary late effects service so patients don't feel forgotten about after their treatment ends."
Trish has also advocated for the creation of a clinic dedicated to managing the long-term effects of pelvic radiotherapy.
"During my treatment, my GP was a lifeline, kind and willing to help. But after the treatment ended it became painfully clear that the system wasn't built to support the complexity of long-term side effects associated with pelvic radiotherapy and I was left to navigate everything alone,"she said.
She described the emotional toll of coping with incontinence pads, nappies, and vaginal dilators designed to stretch scarred tissue as "devastating."
"My stomach became so swollen from chronic constipation and weight gain that when I looked in the mirror I was looking at someone I no longer recognised,"Trish added.
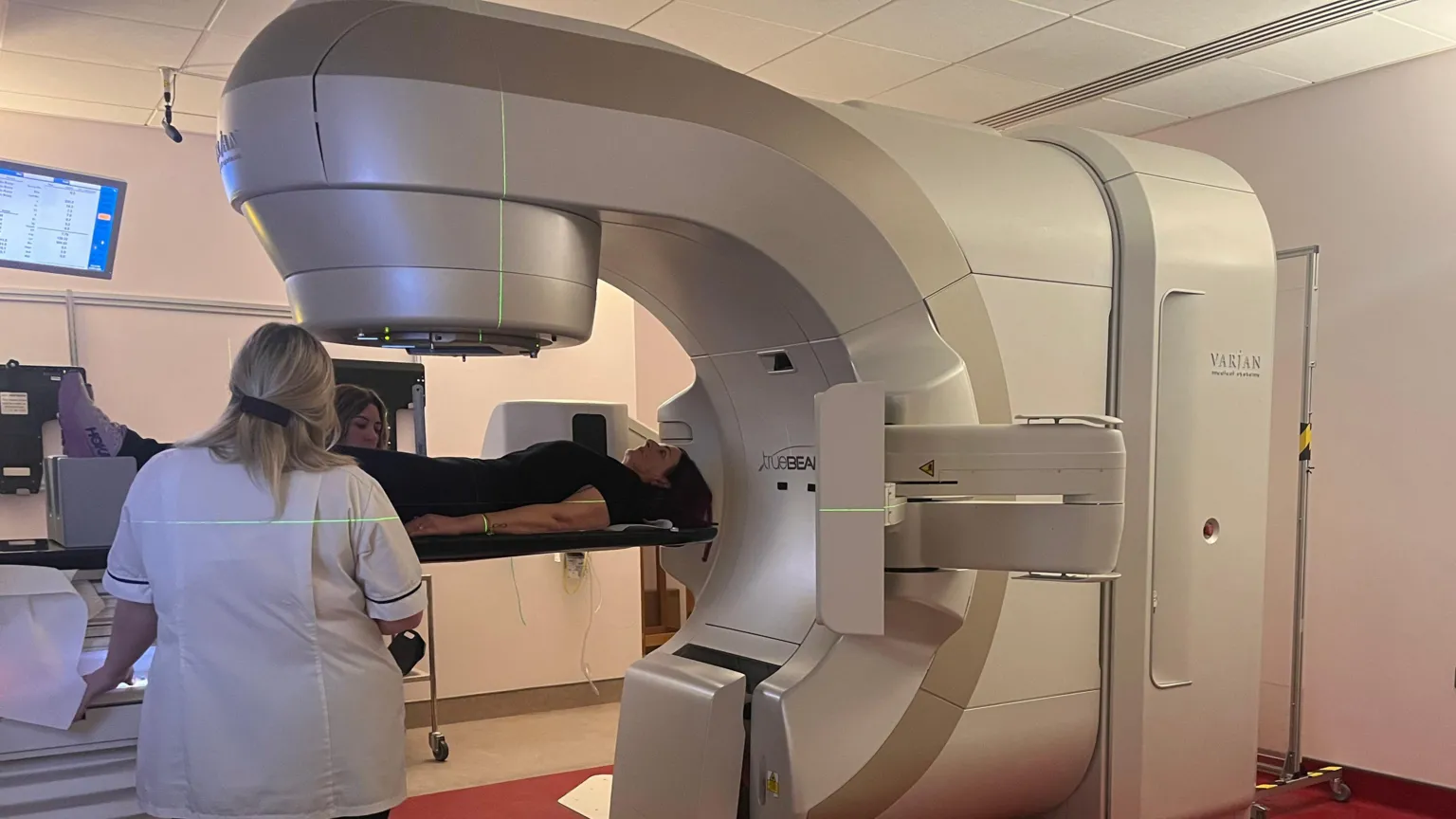
Physical and mental scars
This weekend marks the first event in Northern Ireland dedicated exclusively to raising awareness of anal cancer, involving patients, clinicians, and charities.
Alison Irwin, a clinical nurse specialist at the Belfast Cancer Centre, typically serves as the initial point of contact for patients after treatment.
"It's all about giving them the words and terminology to break the stigma including telling their family and their employer about anal cancer,"she said.
"It's vital that patients feel they can open up to us and tell us everything about their bodies; I have heard it all before, so my relationship with the patient is important,"Irwin added.
Dr Catherine Hanna, a consultant clinical oncologist at Belfast Health Trust, emphasized that anal cancer is treatable, particularly when diagnosed early, typically through radiotherapy.
"It is a rare cancer, and people should look out for a lump in the area, itching and even bleeding.
If someone is noticing something different in their body, they should get it checked out,"she said.







