Tragic Loss of Bethan James
When she was 16, Bethan James shared on her YouTube channel that by 2026 she hoped to have a partner, an enjoyable job, and possibly children.
Bethan would have been 27 years old now, but her life was cut short when she died at 21 from a combination of sepsis, pneumonia, and Crohn's disease.
Bethan's sepsis was not identified early enough, delaying critical care. Her grieving parents are now advocating for improved training to better diagnose sepsis, one of the UK's leading causes of death.
A BBC investigation revealed that sepsis awareness training is still not mandatory in most Welsh hospitals, raising concerns from Bethan's parents that similar tragedies could occur again.
The hospital where Bethan passed away and the Welsh government stated that sepsis awareness remains a focus and priority, while the Welsh Ambulance Service reported that "meaningful changes" have been implemented.
"She was just the kindest, most caring, loving person and she had so much to give," said Jane James, Bethan's mother, from Cardiff.
"It just pulls at your heartstrings thinking, where would Bethan be today and what would she be doing? We still go about daily things, but underneath there's just this total devastation and so many dark, dark moments. It's a totally abnormal life we live," added Steve James, a former England cricket international and Bethan's father.

Understanding Sepsis and Its Impact
Sepsis occurs when the body's immune system overreacts to an infection, attacking its own tissues and organs.
The UK Sepsis Trust estimates approximately 48,000 deaths annually in the UK are related to sepsis, with thousands deemed preventable.
Bethan died six years ago this week. Her parents campaigned for an inquest, where a coroner concluded that Bethan "would not have died" if her treatment had not been delayed.
A BBC investigation found that sepsis awareness training remains inconsistent across Wales and is not compulsory at the University Hospital of Wales in Cardiff, where Bethan died.
"You go into the hospital and there's sepsis posters on lifts and walls but if their actual frontline staff can't recognise the symptoms of sepsis, it just beggars belief," said Jane.

Hospital Visits and Missed Diagnoses
In the ten days before her death, Bethan was unwell and made five visits to hospital.
"They were just quite dismissive of her symptoms," Jane, a physiotherapist, said. "Her heart rate was high, her blood pressure was low - it was so hard to get them to listen."
Bethan's condition deteriorated, and she returned to hospital days later, seeing the same doctor.
Steve, now a sports writer for The Times, recalled a medic telling them Bethan would recover soon.
"I was due to go to Ireland to cover the Six Nations rugby game between Ireland and Wales," Steve said. "I was unsure whether to go but [I remember] him saying that he thought she would be OK in two weeks' time."
"Even on the Saturday when she died, [Bethan] kept saying to Jane 'that doctor said I was going to be OK'. I went to Ireland. That's a decision I've got to live with the rest of my life - I regret it so deeply, but I just took his word."

Rapid Decline and Emergency Response
A day after Steve left for Dublin, Bethan's condition worsened. Jane called 999, and a paramedic arrived at their Cardiff home.
"She had a temperature, she looked grey, she was cold, and she had pain in her chest," Jane recalled. "We found out later that they couldn't record her blood pressure because it was so low. All of those symptoms were a red flag for sepsis."
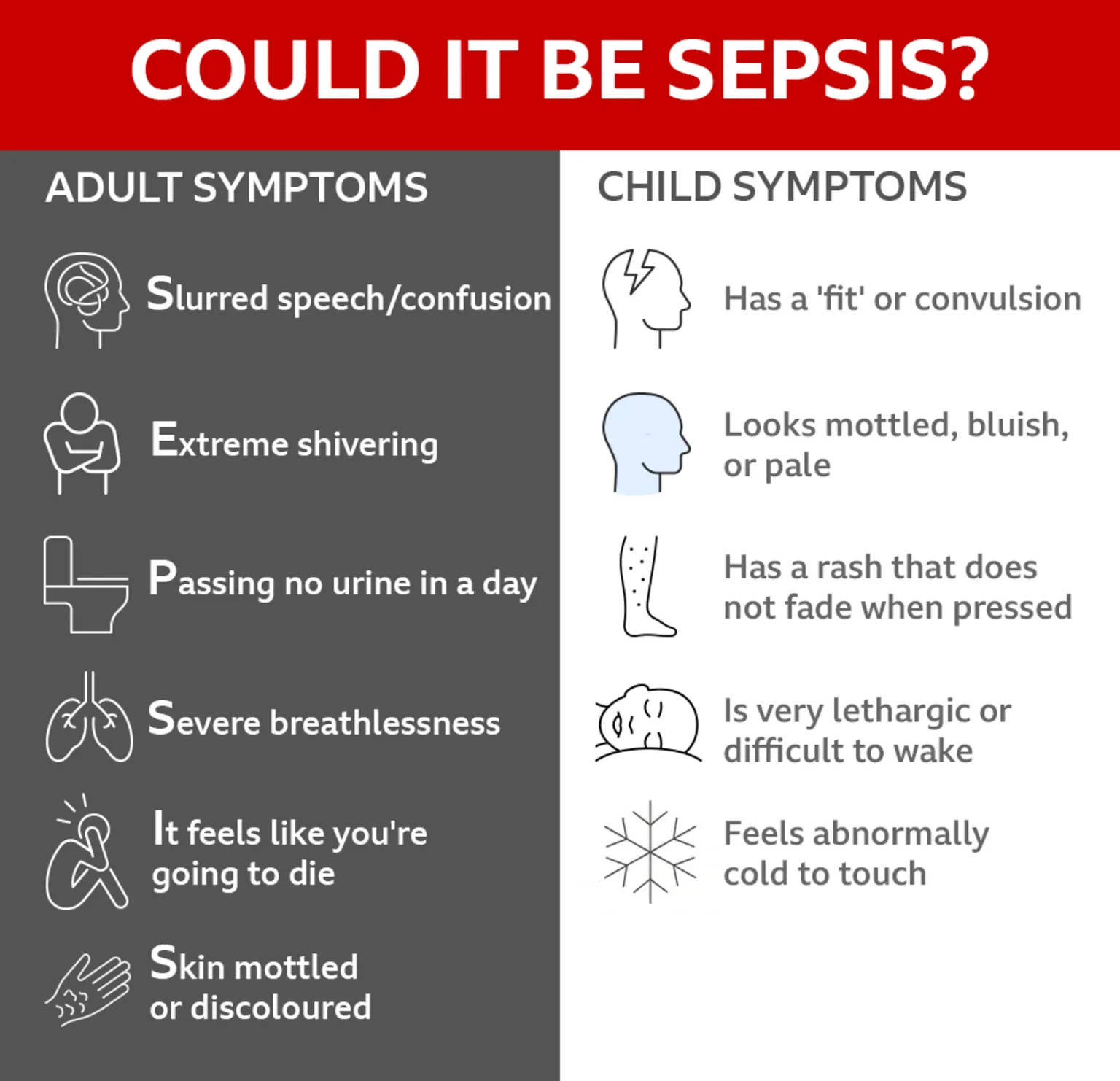
Bethan was assessed and given a National Early Warning Score (NEWS), which evaluates blood pressure, heart rate, and breathing rate.
A NEWS score above seven indicates a severe risk of sepsis requiring urgent emergency medical review.
Bethan's NEWS score was eight, but the paramedic did not recognize the possibility of sepsis.
Although an ambulance was called, Bethan was not prioritized, and the hospital was not forewarned. Upon arrival around 20:00 GMT, there was no resuscitation bed prepared for her.
"A&E that night was chaos, there was no-one taking overall care of Bethan," Jane said. "She was so unwell, her blood pressure was so low, her lips were going blue, she was all blotchy, she was breathing really fast to try and get air in. The nurse that triaged her should have known that it was sepsis with a NEWS score of eight."
Almost an hour after admission, Bethan was transferred to the resuscitation unit where tests confirmed sepsis, and she was administered antibiotics. However, it was too late.
"The doctor said to Bethan 'we think you've got sepsis'," Jane recalled. "That's the last thing she heard. They asked me to leave. She had a cardiac arrest about five minutes later and died at 22:00."
Steve rushed back from Dublin but did not arrive in time. He was informed of Bethan's death while driving home on the M4 from Heathrow airport.

Responses from Health Services
The Welsh Ambulance Service apologized for the "errors identified in Bethan's case" and stated that sepsis training is now mandatory, with "meaningful changes" implemented.
Cardiff and Vale University Health Board, which manages the University Hospital of Wales, said that "sepsis awareness and early recognition are priorities" and that it is "continuously reviewing sepsis training to improve consistency and accessibility."
A BBC Freedom of Information request to all Welsh health boards found that where mandatory training exists, it is included within other modules rather than as standalone sepsis training.
The BBC also found inconsistent auditing of training completion, with some health boards not recording completion rates at all.
"It's absolutely shocking," said Dr Ron Daniels, chief medical officer of the UK Sepsis Trust. "This is one of the biggest killers we face. For hospitals not to ensure that their staff are regularly trained is almost negligent. It's letting people die because their staff are not trained, but they also perceive that their organisation doesn't take this condition seriously."
Calls for Mandatory Sepsis Training
The UK Sepsis Trust advocates for mandatory standalone sepsis awareness training for all clinical hospital staff to ensure early detection.
"For every hour we delay giving life-saving treatment, the patient's chance of survival falls," Dr Daniels said. "In rapidly progressing cases like Bethan's, that's even more time critical."
Initiatives and Gaps in Wales and England
The BBC's research revealed that Aneurin Bevan University Health Board in south-east Wales has introduced a scheme called Call for Concern, allowing staff, patients, families, and carers to request a second opinion when inpatients' conditions deteriorate rapidly.
This scheme has been partially implemented in three other Welsh health boards, with the remaining three planning future adoption. However, outpatient areas such as A&E units are excluded.
In England, families can request urgent second opinions in all hospital areas, including A&E, through Martha's Rule, named after 13-year-old Martha Mills who died in 2021 due to missed sepsis treatment opportunities.
Bethan's parents and the UK Sepsis Trust have urged for the introduction of Martha's Rule or a similar protocol in Wales, covering A&E departments as well.
Ambulance Services and Pre-Hospital Antibiotics
The National Institute for Health and Care Excellence (NICE) recommends that ambulance services administer antibiotics in sepsis cases where combined transfer and handover times to hospital emergency departments exceed one hour.
The BBC surveyed ambulance trusts across the UK regarding adherence to these guidelines. Only Scotland and the Isle of Wight confirmed full compliance, with South Central Ambulance Service in southern England partially implementing the recommendation.
The UK Sepsis Trust urges other ambulance services to follow the examples of Scotland and the Isle of Wight and comply with NICE guidelines.
"I would argue that pretty much every ambulance service's transit times are more than an hour so we should be giving pre-hospital antibiotics," Dr Daniels said.
"If we lived in the Isle Of Wight, Bethan would be alive," Steve said. "That postcode lottery is just so unfair."
Family's Determination for Change
"I think the worst thing is that I know she could have survived if she had the right treatment. I don't want any other family to go through this - because she should still be here with us. We want changes to be made - and I feel like Bethan's on my shoulder, saying this is what we need to do," Jane said.

The Welsh Ambulance Service expressed openness to further research on the benefits of pre-hospital antibiotic administration by ambulance staff.
Steve and Jane are calling on the Welsh government to mandate standalone, audited sepsis awareness training across all Welsh health boards.
The Welsh government stated that sepsis will be a "focus for NHS Wales improvement plans in 2026-27 to ensure consistent, high-quality care."
"We are taking significant steps to improve how NHS organisations recognise and respond to sepsis, including the use of National Early Warning Scores, new safety information for patients and families, and rolling out Call4Concern in all inpatient wards," a government spokesperson added.






