Personal Struggles Highlight Need for Change
Zoe Trafford, a hairdresser from Liverpool, frequently found herself in the role of confidante for her customers. However, she revealed to the BBC that eventually, the situation reversed, and her salon clients had to listen to her own health challenges.
Zoe has suffered from endometriosis since her teenage years, a condition known to cause intense pain and heavy menstrual bleeding. Despite this, for many years, medical professionals dismissed her symptoms as simply having bad periods.
She initially shared her story with in 2022, coinciding with the release of a women's health strategy for England by the Conservative government.
"You'll be alright, it's just normal,"
she recalled doctors telling her."But it's not normal – I don't think being in pain is normal."
The 2022 strategy aimed to "radically improve" the engagement and responsiveness of the health and care system towards all women and girls, with the goal of enhancing health outcomes.
Four years later, the Labour government is updating this strategy to further address women's healthcare needs.
For Zoe, the past years have brought significant changes, many of which have negatively impacted her life. She underwent major surgery involving the removal of her womb and part of her bowel, and she now manages her bladder by self-catheterization.
Despite these interventions, she feels unheard within the healthcare system.
"I'm not being listened to. Basically, I've had the surgery but I'm having more and more complications,"
Zoe has had to cease working as a hairdresser because the pain from standing is unbearable. She describes an ongoing cycle of referrals without resolution.
"I'm being passed from urology to 'gynae' back to the GP, and it's just like I'm in a vicious circle, and no one seems to know what to do with me now,"
she said.
'The system is failing women'
The updated women's health strategy is being introduced amid widespread criticism that the NHS often marginalizes and ignores women's voices.
Health Secretary Wes Streeting acknowledged these issues, stating that some women have felt like "second class citizens" with their pain dismissed as "an inconvenience" and their symptoms regarded as "an overreaction."
"It's clear the system is failing women,"
he said.
Supporting this assertion, BBC analysis reveals a dramatic increase in the number of women waiting for gynaecological procedures in England. Between February 2020 and January 2026, the waiting list doubled to over half a million (565,000).
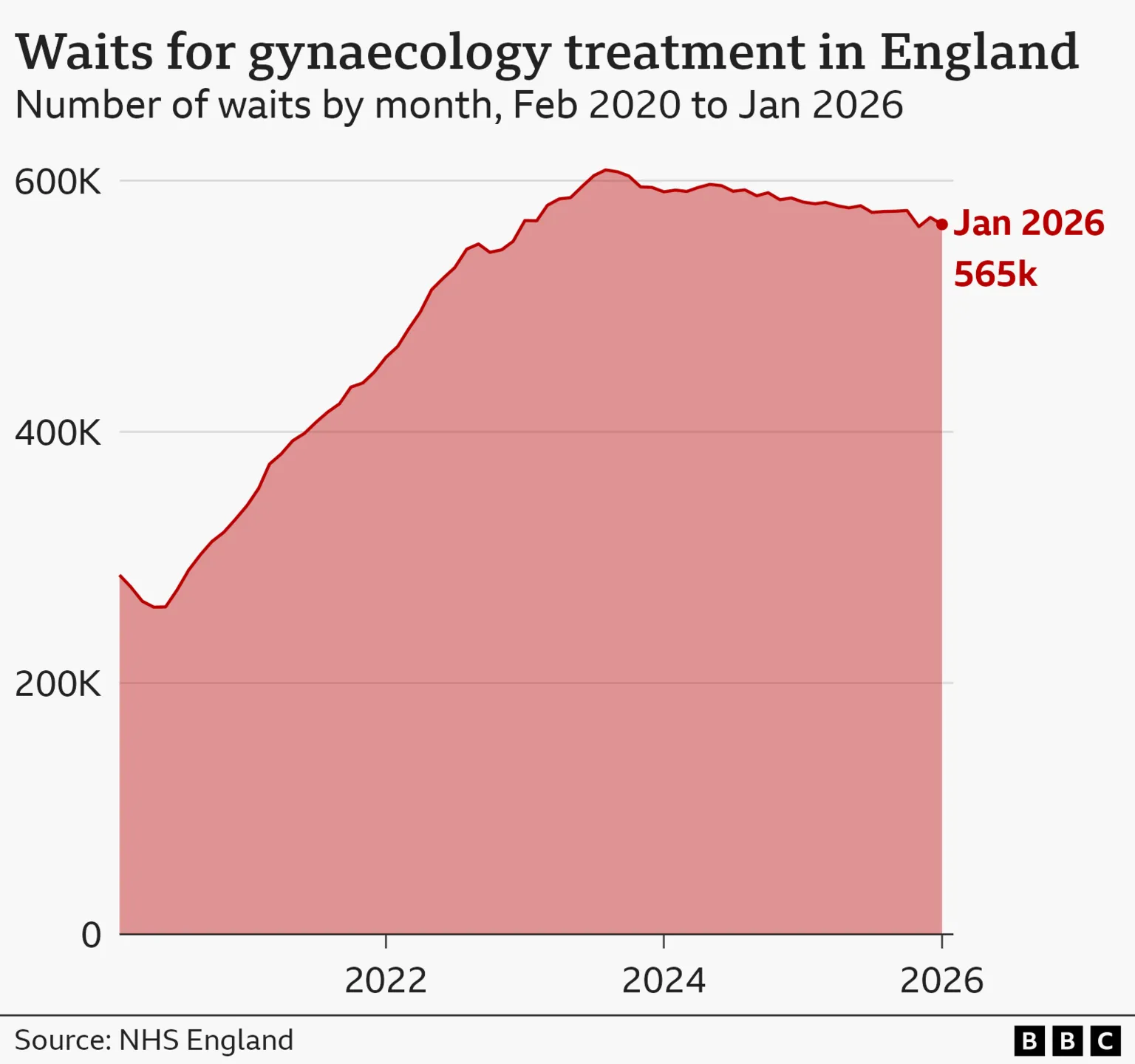
While waiting lists for other planned treatments (excluding mental health) have also risen, the increase was smaller at 58%.
Among the new initiatives announced by the government is a "patient power payment" scheme. This program will allow women to provide feedback and report their treatment experiences. Funding will then be directed towards areas requiring improvement, and providers receiving poor feedback may face financial penalties.
Gynaecology has been chosen as the first specialty to trial this scheme, with potential expansion to other health conditions in the future.
The strategy also includes plans to streamline referrals to appropriate clinicians to reduce long waiting times for treatment.
Additionally, a new standard of care will be introduced to ensure women receive adequate pain relief during invasive gynaecological procedures.
Dr Alison Wright, president of the Royal College of Obstetricians and Gynaecologists, expressed cautious optimism about the strategy but highlighted ongoing concerns.
"With over 565,000 women still waiting for gynaecological care, there is a clear opportunity to embed Women's Health Hubs within the neighbourhood health model,"
she said.
The Royal Osteoporosis Society raised questions about the strategy, noting the absence of a national plan for specialist services addressing osteoporosis. This condition affects half of women over 50 and increases their risk of hip fractures, despite previous government commitments.
Dr Sarah Jarvis, a GP and ambassador for the Royal Osteoporosis Society, emphasized the urgency.
"Around 2,000 lives were at stake every year without a clear plan,"
she said.
Emma Cox, chief executive of Endometriosis UK, described the new strategy as "desperately needed." She criticized the prolonged diagnosis times for endometriosis, which can exceed nine years.
"These commitments must be matched with a clear roadmap for delivery, including ensuring the necessary resources and capacity,"
she added.
Regional Developments in Women's Health
In Scotland, the government recently published phase two of its women's health plan, initially launched in 2021. This phase focuses on transforming services to provide timely access to gynaecological care for women and girls.
The Welsh government introduced a Women's Health Plan in 2024 aimed at closing the gender health gap by enhancing health services for women.
Meanwhile, authorities in Northern Ireland have been developing a Women's Health Action Plan to address similar concerns.






