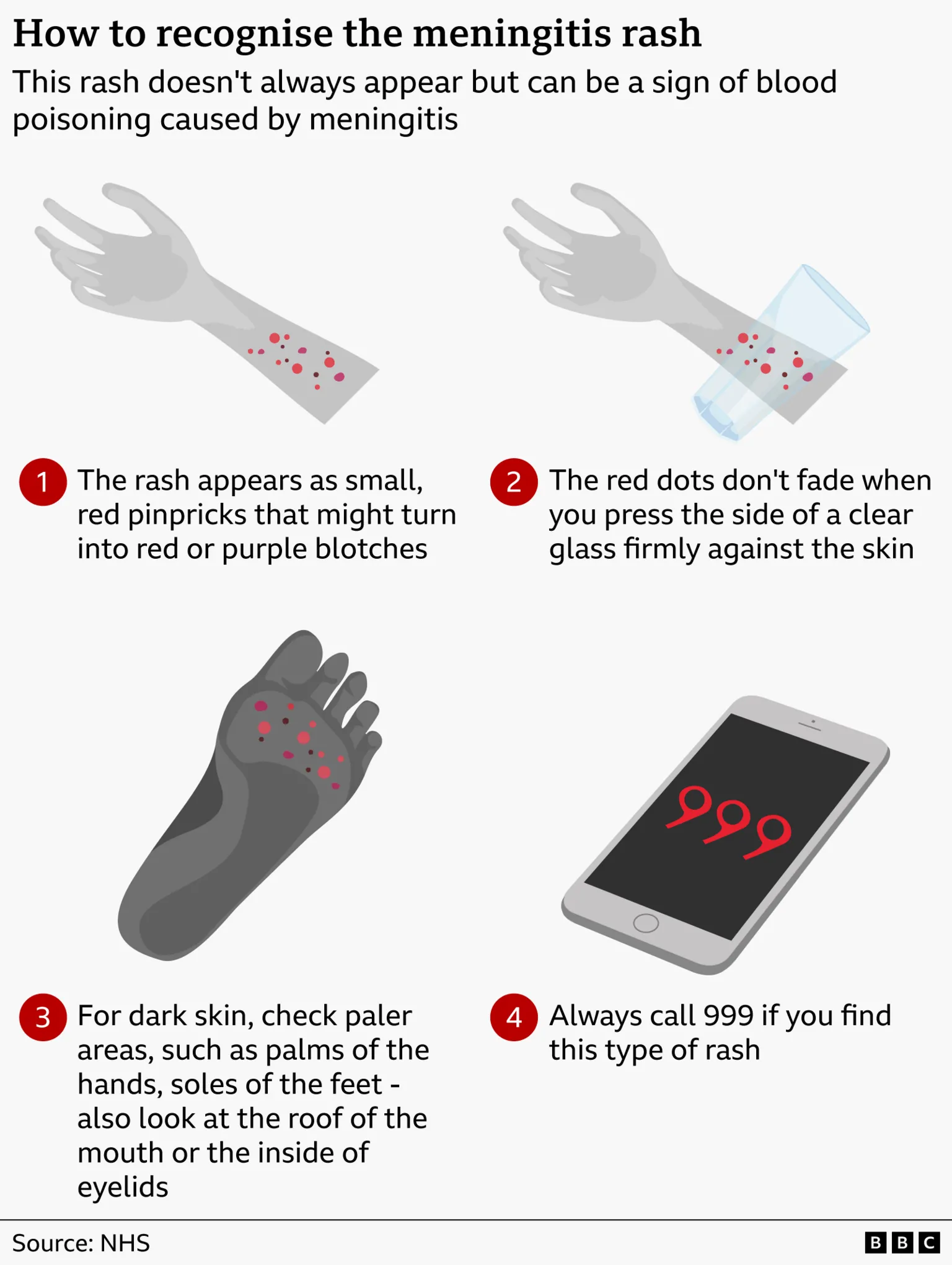
A meningitis outbreak in Kent has been associated with a strain against which most teenagers lack protection.
Two fatalities have been confirmed: a 21-year-old university student and an 18-year-old school pupil.
The UK Health Security Agency (UKHSA) has reported two additional meningitis cases in the Canterbury area of Kent, raising the total to 15. All affected individuals have been hospitalized, with four cases confirmed as meningitis B infections.
The majority of young people born before 2015 have not received the meningitis B vaccine unless they obtained it privately. Authorities are urging hundreds of people to take antibiotics to help prevent further spread of the infection.
Health experts Dr Ellie Cannon, a general practitioner, Dr Tom Nutt, chief executive of the charity Meningitis Now, and the BBC's health editor Hugh Pym have been responding to public inquiries regarding the outbreak.
How is meningitis transmitted?
Hugh Pym explained that meningitis can be transmitted through "close personal contact." This transmission is more likely in crowded environments or close living quarters.
"It can also be spread by people who are not presenting with symptoms,"he noted.
He added that while meningitis is not as contagious as illnesses like influenza or Covid-19, it can deteriorate rapidly.
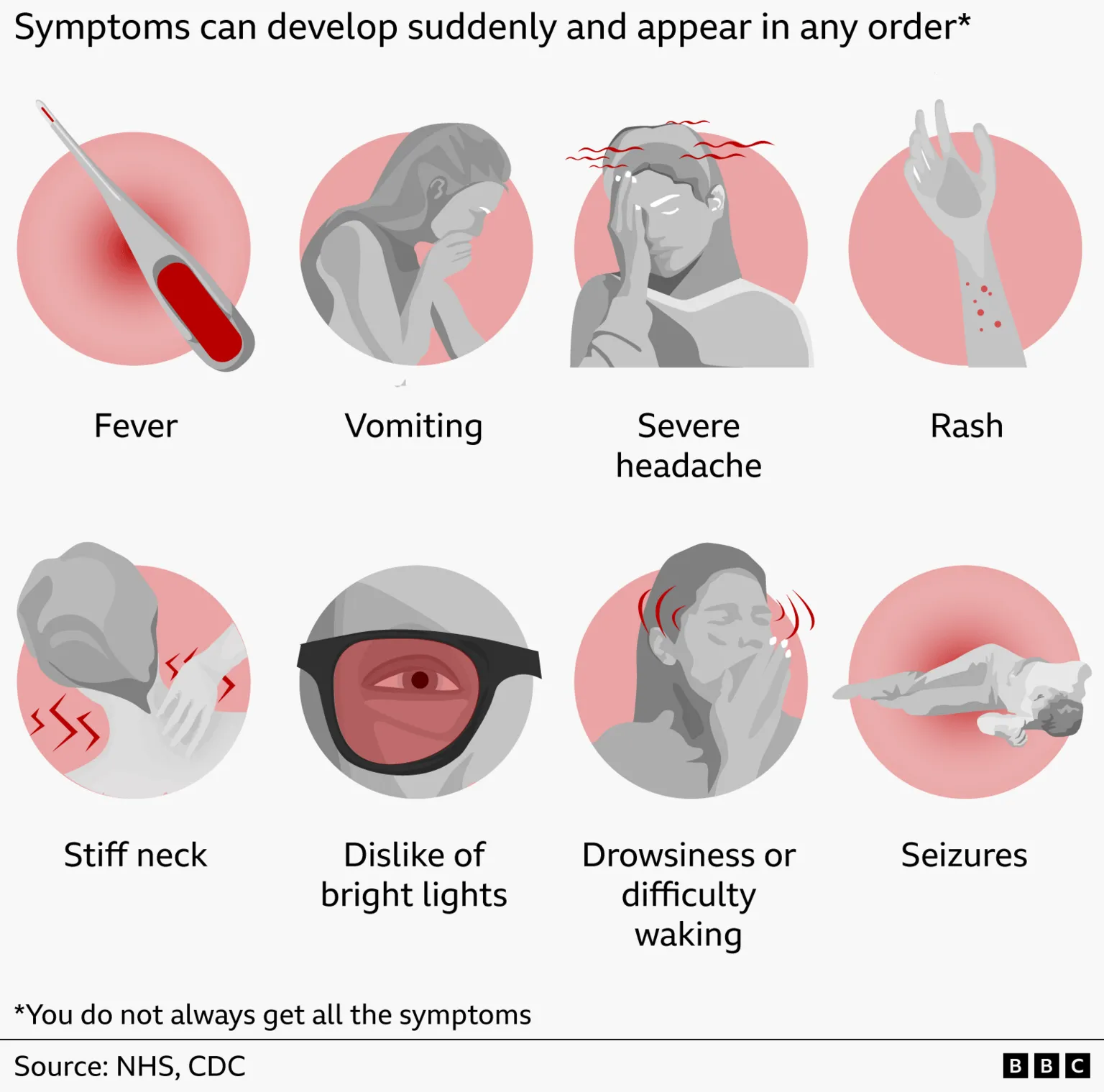
Are only children born after 2015 vaccinated for Meningitis B?
Dr Ellie Cannon clarified that the meningitis B vaccine was introduced for babies born on or after 1 July 2015.
"That means it is very possible teenagers now will not have received it because that was not on the schedule when those young adults were babies,"she said.
She added that some young people may have received the vaccine privately.
Another vaccine, MenACWY, which protects against four strains of meningococcal bacteria, is offered to teenagers at school around ages 13 or 14. However, this vaccine does not protect against meningitis B.
"The concern right now is therefore about young adults not having had the meningitis B vaccines and this is what parents should be checking,"Cannon emphasized.
How serious is meningitis?
Dr Tom Nutt described meningitis as a disease that can cause "devastation when it strikes," with approximately one in ten people infected by bacterial meningitis dying.
"It is not unusual for people to die within 24 hours or less,"he added.
"There is something particularly nasty about this disease, which causes untold pain to families,"Nutt stated.
Why is meningitis spreading now?
Nutt explained that meningitis outbreaks have a "tragic randomness" and are unpredictable.
"There's a necessary vigilance that's required all the time,"he said.
Given the rapid progression of meningitis, he stressed the importance of individuals informing their flatmates or neighbors if they feel unwell so others can monitor their condition.